Over the last year or so, I have really delved into the research literature on tendinopathy assessment and treatment. This was motivated in part thanks to an excellent continuing education course that I took from tendinopathy expert Dr. Peter Malliaras, PT, PhD called: “Mastering Lower Limb Tendinopathy 2nd Edition.”1 I have also been interested in this research because of the high number of patients that I was working with this spring who were experiencing tendinopathy related injuries.
These next few blog posts will explore some of what I have learned in trying to provide the best evidence-based and effective care to patients with lower extremity tendinopathies. In each post, I will try to weave together the research basis for evaluation and treatment decisions as well as clinically relevant tips. Here is what you can expect:
Part 1: Tips for Treating Lower Extremity Tendinopathies: ASSESSMENT
Part 2: Tips for Treating Lower Extremity Tendinopathies: EXERCISE PRESCRIPTION
Part 3: Tips for Treating Lower Extremity Tendinopathies: INDIVIDUALIZING TREATMENT (CASE EXAMPLES)
See Below for Part 1…
Part 1: Tips for Treating Lower Extremity Tendinopathies: ASSESSMENT
Tendons play a key role in producing movement from our bodies. They connect muscle to bone and in synergy with muscle contraction, tendons serve to:
- Transmit forces
- Provide a mechanism for energy storage and release
- Optimize the length-tension relationship of muscles as they work as force generators
When tendons are working well, they help us engage in movements that utilize this “stretch-shortening” cycle of loading a muscle-tendon unit, such as running, jumping, and walking.2
However, tendons can be prone to overuse injuries from repetitive trauma.3 Commonly, tendon injuries occur when an individual changes his or her training load too quickly or too drastically. This can range anywhere from a large increase in running mileage, footwear changes, adding more speed work, or even an increase in the amount of walking a person may be doing. All of these changes can alter the load felt by the tendon and can lead to changes at the tendon tissue level. “Pathological” tendons (aka tendons afflicted by “tendinopathy”) often demonstrate predictable structural changes in in various aspects of the tendon including tendon cells, collagen, and components of the extra-cellular matrix.4
These changes can include4:
- Signs of inflammation and/or degeneration
- Neovascularization and nerve ingrowth
- Disorganized collagen and an increase in weaker type collage (type III)
- Reduced number of fibroblasts
- Extracellular matrix changes
When evaluating a patient with a suspected tendinopathy, it is important to rule out other diagnoses and once the clinical diagnosis of tendinopathy is decided upon, it is important to “stage” that individual based on acuity or irritability of the tendon (i.e., How painful is it? How little load does it take to bring on pain?). This staging allows you as the treating clinician to better optimize healthy loading to the tendon and to prescribe appropriate exercises and adjunct treatments.
As you evaluate a patient with a suspected tendinopathy, here are some signs and symptoms that are common to tendinopathy and aspects that you will want to look out for in your clinical exam (also, can help provide evidence for your working diagnosis of tendinopathy):
TENDINOPATHY SUBJECTIVELY
- Localized pain at the tendon
- Pain is proportional to loading (for example more walking leads to more pain)
- Pain is provoked with high/fast loads (for example running makes the tendon hurt more than walking)
- The Tendon “warms up”, or feels better once into an activity (for example 5-10 min into a run, pain goes away or intensity is diminished…)

TENDINOPATHY OBJECTIVELY
- Weak and painful at the affected muscle-tendon unit5
- Pain with active contraction and passive stretch
- Assess load tolerance and irritability
- If LOW irritability > it may take HIGH load or reps to reproduce pain!
- If HIGH irritability > LOW loads will reproduce pain (light stretch, AROM, MMTs)
- Offloading the tendon can reduce pain & symptoms
- This can be diagnostic and serve as a treatment (e.g., heel lift for Achilles’ tendinopathy, orthotics or night splint for plantar fasciitis)
- Palpation pressure at the tendon will likely reproduce pain
- Tendinopathy “Special Tests” (from low to high load- use in exam based on irritability):
- Achilles’ Tendinopathy: bilateral heel raise <> unilateral heel raise <> single leg hop
- Posterior Tibialis Tendinopathy: same as above
- Plantar Fasciitis: same as above
- Patellar Tendinopathy: loaded knee extension <> jumping or running
- Gluteal Tendinopathy: walking <> single leg stance <> step up onto high step
- High Hamstring Tendinopathy: active straight leg raise <> straight leg raise + overpressure
*Other Factors for a comprehensive evaluation:
- Assess joints above and below for mobility and strength impairments
- Assess functional lower extremity movements and movement patterns
From your evaluation you will want to stage the patient’s load tolerance and the irritability of the tendon. This staging is based on pain and symptoms with loading and will be very important in guiding your prognosis and treatment plan…
…more on STAGING & TREATMENT BASED ON ACUITY in Part 2!
TREATMENT PREVIEW:
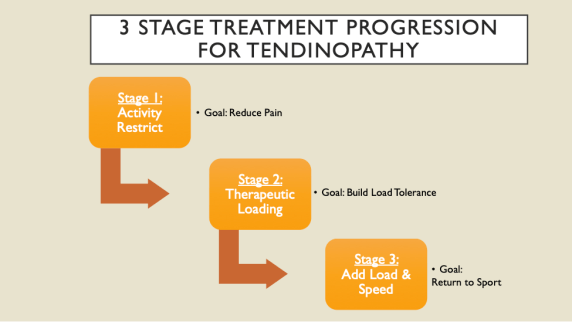
Check Out Parts 2 and 3 here:
Part 3: INDIVIDUALIZING TREATMENT (CASE EXAMPLES)
References:
- Malliaras P. Mastering Lower Limb Tendinopathy 2nd https://www.tendinopathyrehab.com/ Accessed: December 18th, 2018
- Clark WH, Franz JR. Do triceps surae muscle dynamics govern non-uniform Achilles tendon deformations? PeerJ. 2018; 6:e5182.
- Malliaras P, Barton CJ, Reeves ND, Langberg H. Achilles and patellar tendinopathy loading programmes: A systematic review comparing clinical outcomes and identifying potential mechanisms for effectiveness. Sports Medicine. 2013; 43(4):267-286.
- Magnusson SP, Langberg H, Kjaer M. The pathogenesis of tendinopathy: balancing the response to loading. Nature Reviews Rheumatology. 2010; 6(5): p. 262-268.
- Cyriax J. Textbook of orthopaedic medicine, diagnosis of soft tissue lesions, vol 1, 8th edition. London: Baillière Tindall; 1982.
Grreat share
LikeLike