One of the factors that I love about working in an outpatient orthopedics setting as a physical therapist is the wide variety of patients that walk through the clinic doors. The diversity in age, socioeconomic status, fitness level and goals, and injury type means I am constantly learning and being challenged to identify effective treatments for these individuals. In any given week (or day!), I could work with a competitive collegiate runner with Achilles’ tendinopathy, an older woman with poor balance and general weakness, a chef with carpal tunnel syndrome, and a middle-aged carpenter with lateral elbow pain.
What do all these seemingly very different individuals have in common? I think they could all benefit from exercises geared towards strengthening their feet or hands!
As I read more and seek to integrate exercises targeted at foot strength and grip (hand) strength, I am finding that these two areas are often overlooked by other healthcare providers (including other PTs!) or not prioritized by patients as they seek to get back to playing a sport, performing certain work tasks, or engaging fully in activities of daily living. Exercises targeted at foot strength or grip strength could be used by a physical therapist who can adjust the difficulty, intensity, and dose of the exercises depending on the individuals’ goals and needs.
Why is foot strength so important?
Foot strength and control (i.e., balance/proprioception) could impact an athlete’s ability to create power, literally from the ground up. Many athletes with lower body injuries will have a goal of returning to running or getting back to playing sports involving cutting and jumping. For these individuals, strengthening of foot and ankle muscles could be part of a comprehensive lower body strength program for injuries near the knee or hip or it could be the main focus for athletes with specific foot and ankle injuries. Research suggests that incorporating specific exercises for foot and ankle muscle strength is a key part of rehabilitation for injuries such as lateral ankle sprain (Martin, 2013), chronic ankle instability (Powden, 2019), or Achilles’ tendinopathy (Malliaras, 2013; Martin, 2018; Silbernagel, 2020).
Prioritizing strength in these areas could also prevent an injury from happening in the first place! In one study, runners who went through a foot and ankle muscle strengthening program reduced their risk for running related injuries compared with a group that did not do this training (Matias, 2016; Taddei, 2020).
Note: if you are interested in reading more about lower extremity tendinopathy treatments, I have written extensively about this subject, and you can find some of my blogs on this in the links below:
Tendinopathy Treatment for The Lower Body
Foot strength is also important for basic mobility for older adults. One recent research review suggests that utilizing exercises to improve muscle strength of foot intrinsic muscles could positively impact older adults (defined as age 65 years or older) by allowing them to maintain physical independence and reduce the risk of falls (Futrell, 2022). Falls are a significant issue in an aging population because they can create injuries that may contribute to morbidity and mortality. It could be argued that foot strength can contribute to one’s ability (at any age) to produce power for a movement like a squat. In one study, better lower extremity power such as that needed for repeated sit to stands (i.e., basically body weight squats!) was found to be a robust predictor of physical independence in older adults. (Hetherington-Rauth, 2022).

Why is hand (grip) strength so important?
Improving grip strength and one’s tolerance to activities that use repetitive hand and grip strength is often needed within physical therapy to address hand, wrist, or elbow pain. Specifically, weak and painful gripping activities tend to be characteristic of individuals with, “Tennis Elbow,” (i.e., lateral epicondylalgia) or, “Golfer’s Elbow,” (i.e., medial epicondylalgia). Thus, restoring pain-free gripping is a common goal of physical therapy treatment, and exercises that seek to improve load tolerance of the common extensor (lateral elbow) or common flexor (medial elbow) tendons often comprise a key component of rehabilitation. Also, these conservative treatments (i.e., grip and forearm strengthening, manual therapy, and modalities within physical therapy treatments) are often recommended as first-line, effective treatments compared with more invasive therapies like injections or surgery (Amin, 2015; Chen, 2021; Kim, 2021)

Grip strength can also be a proxy of overall health in older adults. A robust group of research findings indicates that those with better grip strength may live longer (Bohannon, 2019; Celis-Moralis, 2018)!
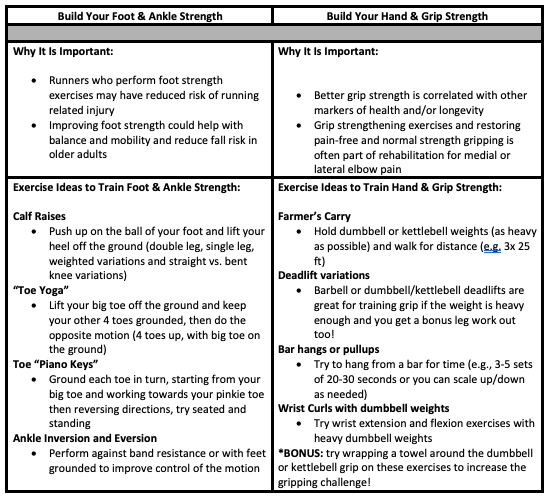
So, how do you build foot strength and grip strength? See Table Below for some ideas!
References:
Amin NH, Kumar NS, Schickendantz MS. Medial epicondylitis: evaluation and management. J Am Acad Orthop Surg. 2015 Jun;23(6):348-55.
Bohannon RW. Grip Strength: An Indispensable Biomarker For Older Adults. Clin Interv Aging. 2019 Oct 1;14:1681-1691.
Celis-Morales CA, Welsh P, Lyall DM, Steell L, Petermann F, Anderson J, Iliodromiti S, Sillars A, Graham N, Mackay DF, Pell JP, Gill JMR, Sattar N, Gray SR. Associations of grip strength with cardiovascular, respiratory, and cancer outcomes and all cause mortality: prospective cohort study of half a million UK Biobank participants. BMJ. 2018 May 8;361:k1651.
Chen Z, Baker NA. Effectiveness of eccentric strengthening in the treatment of lateral elbow tendinopathy: A systematic review with meta-analysis. J Hand Ther. 2021 Jan-Mar;34(1):18-28.
Futrell EE, Roberts D, Toole E. The effects of intrinsic foot muscle strengthening on functional mobility in older adults: A systematic review. J Am Geriatr Soc. 2022 Feb;70(2):531-540.
Hetherington-Rauth M, Magalhães JP, Alcazar J, Rosa GB, Correia IR, Ara I, Sardinha LB. Relative Sit-to-Stand Muscle Power Predicts an Older Adult’s Physical Independence at Age of 90 Yrs Beyond That of Relative Handgrip Strength, Physical Activity, and Sedentary Time: A Cross-sectional Analysis. Am J Phys Med Rehabil. 2022 Nov 1;101(11):995-1000.
Kim YJ, Wood SM, Yoon AP, Howard JC, Yang LY, Chung KC. Efficacy of Nonoperative Treatments for Lateral Epicondylitis: A Systematic Review and Meta-Analysis. Plast Reconstr Surg. 2021 Jan 1;147(1):112-125.
Malliaras P, Barton CJ, Reeves ND, Langberg H. Achilles and Patellar Tendinopathy Loading Programmes: A Systematic Review Comparing Clinical Outcomes and Identifying Potential Mechanisms for Effectiveness. Sports Medicine. 2013;43(4):267-286.
Martin RL, Davenport TE, Paulseth S, Wukich DK, Godges JJ. Ankle Stability and Movement Coordination Impairments: Ankle Ligament Sprains: Clinical Practice Guidelines Linked to the International Classification of Functioning, Disability and Health From the Orthopaedic Section of the American Physical Therapy Association. J Orthop Sports Phys Ther. 2013;43(9):A1-A40.
Martin RL, Chimenti R, Cuddeford T, et al. Achilles Pain, Stiffness, and Muscle Power Deficits: Midportion Achilles Tendinopathy Revision 2018: Clinical Practice Guidelines Linked to the International Classification of Functioning, Disability and Health From the Orthopaedic Section of the American Physical Therapy Association. Journal of Orthopaedic & Sports Physical Therapy. 2018;48(5):A1-A38.
Matias AB, Taddei UT, Duarte M, Sacco IC. Protocol for evaluating the effects of a therapeutic foot exercise program on injury incidence, foot functionality and biomechanics in long-distance runners: a randomized controlled trial. BMC Musculoskelet Disord. 2016 Apr 14;17:160.
Powden CJ, Hoch JM, Jamali BE, Hoch MC. A 4-Week Multimodal Intervention for Individuals With Chronic Ankle Instability: Examination of Disease-Oriented and Patient-Oriented Outcomes. J Athl Train. 2019 Apr;54(4):384-396.
Silbernagel KG, Hanlon S, Sprague A. Current Clinical Concepts: Conservative Management of Achilles Tendinopathy. Journal of Athletic Training. 2020;55(5):438-447.
Taddei UT, Matias AB, Duarte M, Sacco ICN. Foot Core Training to Prevent Running-Related Injuries: A Survival Analysis of a Single-Blind, Randomized Controlled Trial. Am J Sports Med. 2020;48(14):3610-3619.
This is all very insightful and informative! Thank you for sharing this post Dr. McDaniel. I agree that we can all stand to strengthen our feet and hands, for some of the benefits you cited as well as countless others. A Strength and Conditioning professor at my undergraduate would often say “you’re as strong as your weakest link” and this applies with feet and hands for sure. I already practice some of the exercises you mentioned and intend to integrate the others into my daily movement practice.
I have also found yoga to be very helpful in strengthening hands/wrists and foot/ankle as well as improving proprioception and proximal joint stability/engagement. I went bouldering yesterday and it was a clear and humbling reminder that my grip could use some strengthening and improved endurance. I will be shifting my focus to that end as I feel pretty satisfied with my foot and ankle health because of what I’ve done over the past few years. Thanks again for sharing what you’ve learned in such a digestible and practical format! Looking forward to future posts.
LikeLike